The debate between SOAP and DAP notes is largely academic for most Irish consultants. What matters is whether your documentation workflow is fast enough to survive a 25-patient clinic, structured enough to survive a VHI audit, and good enough to generate a clinic letter in under two minutes.
Most practice management tools were designed by people who have never run a private clinic. The note format was an afterthought. Let's fix that.
Why Documentation Is a Revenue Problem, Not Just a Compliance One
Poor clinical documentation in private practice doesn't just create medicolegal risk — it directly hits your bottom line. A poorly structured operative note delays your insurance claim. A missing diagnosis code means a rejection. A clinic letter that takes three days to generate damages your referral relationship with the GP.
Structured notes, done right, are the backbone of a high-functioning private practice. The format you choose should serve your billing workflow, your GP correspondence, and your clinical thinking — in that order of practical urgency.
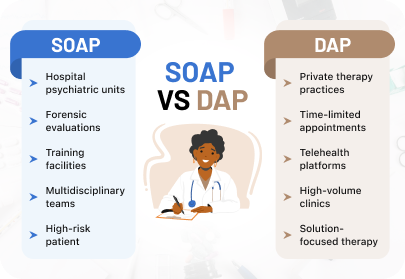
SOAP Notes: The Familiar Standard
Subjective → Objective → Assessment → Plan
Most of us learned SOAP in medical school and it's genuinely well-suited to complex consultant-level cases — particularly in surgical specialties where the distinction between what the patient reports and what you find on examination carries real diagnostic and medicolegal weight.
Where SOAP works well for Irish consultants:
- Complex multi-system presentations where separating patient-reported symptoms from objective findings matters
- Cases likely to end up before the Medical Council, insurers, or in litigation — the structured paper trail is your friend
- Multidisciplinary contexts where allied health professionals are also documenting in the same record
- Surgical specialties where the operative note needs to map cleanly to the insurance claim
The honest limitation: SOAP notes take longer to complete. In a 30-patient private clinic, that time compounds quickly. If your PMS isn't auto-populating fields, carrying forward relevant history, and structuring the note intelligently, you're just adding admin overhead to an already long day.
DAP Notes: Faster, But Know When to Use Them
Data → Assessment → Plan
DAP collapses the subjective/objective distinction into a single Data field. For many consultants — particularly in outpatient follow-up, where you know the patient, the history is established, and you're primarily tracking progress — this is the more efficient format.
Where DAP works well for Irish consultants:
- Routine follow-up appointments where re-documenting full subjective/objective detail adds no clinical value
- High-volume outpatient clinics where documentation speed is the primary constraint
- Specialties with a strong therapeutic or monitoring focus, where the patient interaction itself is the "data"
The honest limitation: DAP notes can be too lean for new patient assessments, surgical workups, or any case where you need to demonstrate clearly how you arrived at your diagnosis. In the Irish private insurance context — VHI, Laya, Irish Life — claims reviewers want to see a logical clinical trail. DAP doesn't always provide it.
The Real Question: Is Your PMS Working Against You?
The format debate is secondary to the tooling problem. If your current system doesn't support flexible documentation templates, doesn't auto-generate clinic letters from your notes, and doesn't feed your documentation into the billing module, then the note format is the least of your problems.
What you should be asking:
- Does my note auto-populate the patient demographic and referral data from HealthLink?
- Does my operative note directly feed the insurance claim, or am I re-keying procedure codes manually?
- Can I dictate a clinic letter from the same note structure and have it ready to send via Healthmail before the patient reaches the car park?
If the answer to any of those is no, you have an infrastructure problem, not a documentation format problem.
What We Built in Enquiry Medical
When I built Enquiry Medical, I wasn't trying to solve a note format problem. I was trying to solve a Tuesday evening problem — sitting in an empty clinic at 8pm finishing letters that should have been done by 6. The note format was irrelevant. What mattered was whether the system turned my clinical thinking into a letter, a claim, and a HealthLink dispatch automatically. That's what we built.
The goal isn't to pick the perfect note format. The goal is to walk out of clinic with your documentation done, your letters sent, and your claims submitted — without a three-hour admin session the following morning.
That's what practice management software should do. For too long, Irish consultants have accepted less.
Enquiry Medical is a practice management platform built by a consultant, for consultants. If you'd like to see how it handles clinical documentation in your specialty, book a 30-minute demo.

 No hidden fees | Scale your practice with clear pricing and packages →
No hidden fees | Scale your practice with clear pricing and packages →